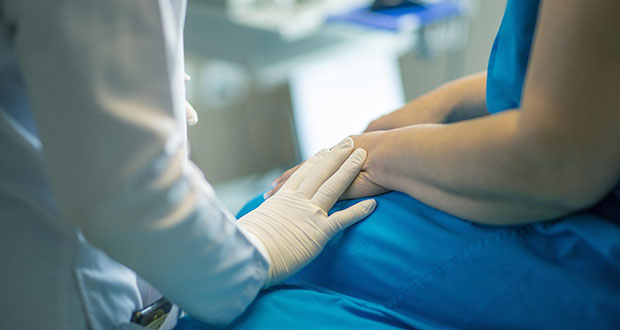
As countries around the globe enforce social distancing and self-isolation to fight the COVID-19 pandemic, telehealth is emerging as a critical tool to connect physicians and other healthcare professionals with patients dealing with chronic cardiovascular conditions.
“Before this pandemic, telehealth or telemedicine was sort of an ‘top of the cake’ kind of a situation for the vast majority of healthcare facilities, at least in the cardiology space,” Andrew Freeman, MD a member of the ACC Health Care Innovation Council, said that. “This has actually been a blessing in a very awful disguise in that we now have an enormous impetus to do this and do it well. But that being said, what that looks like is very rapidly changing.”
Check: Reforming Health Care Systems.
Telemedicine is a broad term describing the provision of healthcare to patients virtually, whether that be over an institutional video conferencing program, a more commercial application like FaceTime or Skype, or even simply via telephone. With the current public health crisis, the Centers for Medicare and Medicaid Services and the Food and Drug Administration have each loosened prior to telehealth restrictions on what physicians, nurse practitioners, and a variety of other providers can offer to their patients and receive reimbursement for. During the height of the COVID-19 outbreak in China, physicians relied heavily on the country’s 5G network to offer telehealth services to patients with nonemergent heart disease.
Some institutions have been offering telehealth services to patients for years now, mostly for rural and disabled patients unable to travel for in-person appointments, but many cardiologists have now been tasked with Transforming their practice almost overnight.
“People need to go in expecting that it's not going to be the same as a face-to-face visit,” In general, the technology is very easy to use and, provided you have an even borderline internet connection, it's quite doable.
The American Heart Association (AHA), which published a primer on telehealth back in 2016, recommended that providers who have never used telemedicine should “opt for basic technologies that allow for real-time video/audio communication and are easy to use for providers and patients alike.
The key is to adopt technology that is affordable, covered by insurance (both public and private), and easy to use.”
As for COVID-19, testing for heart disease onset is essential, as the earlier, it is caught, the easier, and the cheaper, it is to treat. Avoiding long term morbidity becomes the primary goal.
Detecting and diagnosing up to 95% of all common heart diseases including complications resulting from COVID-19 infections. Short of using both and EKG and an Ultrasound (Echocardiograph), there exists no other non-invasive screening and diagnostic medical device that can effectively detect such the onset of such a widespread range of heart disease. Cardio-HART™ it’s ideal for effective Cardiac-Telemedicine™ in the post-pandemic Age of COVID-19.
There are two types of post-pandemic patients, those that manifested overt symptoms of COVID-19 infections, and won, and those that were either infected but asymptomatic or infected but with mild symptoms (and thought it was a simple cold or flu).
Whatever the case, there now exists the real potential for increased risks of COVID-19 infection cardiac implications that could lead to greater numbers and types of heart disease-infected general population.
Telemedicine Primary Care, the new front-line in heart care.
Attacking the disease at its root cause is actually the most effective way to combat CVD.